Paranasal Sinuses
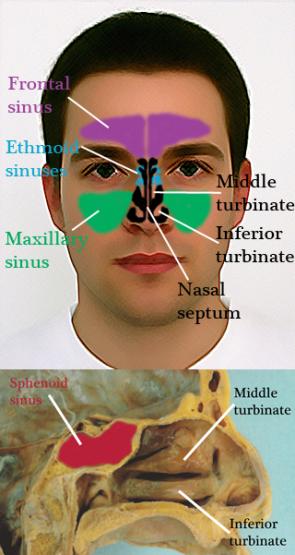 The paranasal sinuses are air-filled extensions of the nasal cavity. They are located in the face/skull and connect directly or indirectly to the nasal cavity and nose through narrow drainage pathways. The frontal sinuses (purple) are located in the forehead region, the ethmoid sinuses (blue) are located between the nasal septum and the eye and just below the brain, and the maxillary sinuses (green) are located in the cheek region below the eyes. The sphenoid sinuses (red) are located behind the ethmoid sinuses and are closely related to important anatomical structures such as the optic nerves that are required for vision, the pituitary gland, and the carotid arteries that carry blood to the brain.
The paranasal sinuses are air-filled extensions of the nasal cavity. They are located in the face/skull and connect directly or indirectly to the nasal cavity and nose through narrow drainage pathways. The frontal sinuses (purple) are located in the forehead region, the ethmoid sinuses (blue) are located between the nasal septum and the eye and just below the brain, and the maxillary sinuses (green) are located in the cheek region below the eyes. The sphenoid sinuses (red) are located behind the ethmoid sinuses and are closely related to important anatomical structures such as the optic nerves that are required for vision, the pituitary gland, and the carotid arteries that carry blood to the brain.
Although there is much debate about the actual purpose of the sinuses they do serve three main functions:
- Resonance of the spoken voice – helps make our pitch and timbre unique
- Protection of surrounding vital structures (crumple-zones)
- Lighten the weight of the skull
Mucus is produced in the nasal cavity and sinuses by the lining called mucosa. Along this mucosa are cells which have small hair-like projections called cilia that push the mucus out of the narrow sinus openings. Other cells help filter the inspired air and prime the immune system. Normally, nasal mucosa produces roughly a cup of mucus a day that is pushed into the back of the nose and eventually swallowed.
Sinusitis is a term that refers to inflammation of the paranasal sinuses, a major health problem in the United States that substantially affects up to 1 in 7 adults. The effects of sinusitis can be disabling in many respects, and have been shown to affect the quality of life, productivity, & finances. Symptoms of sinusitis may include nasal blockage/congestion, facial pain and pressure, nasal drainage, post-nasal drip, and decreased sense of smell and taste. In addition, some patients experience fatigue, headaches, low-grade fevers, tooth pain, eye pressure, and trouble concentrating.
The cause of sinusitis can be infectious or noninfectious. Regardless of the cause, inflammation leads to swelling of the nasal lining and the already narrow openings of the sinuses are made smaller– mucus production is increased and adequate drainage is limited. With long-term swelling and inflammation, the cells of the mucosa are also damaged and cilia can no longer work as effectively. This can lead to a prolonged chronic sinus infection and/or recurrent sinus infections.
Diagnosis:
The diagnosis of sinusitis is based upon a thorough history and physical exam which often includes a diagnostic nasal endoscopy. In addition, radiologic imaging including fine-cut CAT scans are often used to assess the extension and severity of sinusitis. However, this is commonly done only after the patient has completed therapy. The sinusitis is then categorized in one of many different ways. One commonly described method is by the duration of inflammation and symptoms:
- Acute sinusitis is defined as up to 4 continuous weeks of purulent nasal drainage (containing pus) that occurs in the setting of nasal obstruction and/or facial pain or pressure. Most infectious causes of rhinosinusitis are extensions of the viral infection causing the common cold; these typically resolve without medical intervention. However, a minority of these cases progress to infection with bacterial sinusitis and may require treatment.
- Recurrent acute sinusitis is defined as 3-4 or more episodes of acute sinusitis per year without signs or symptoms of infection between episodes.
- Subacute sinusitis is defined as symptoms for more than 4 continuous weeks but less than 12 weeks
- Chronic sinusitis is defined as 12 or more continuous weeks of two or more of the following symptoms:
- purulent (pus-containing) nasal drainage
- nasal obstruction
- facial pain/pressure/fullness
- decreased sense of smell
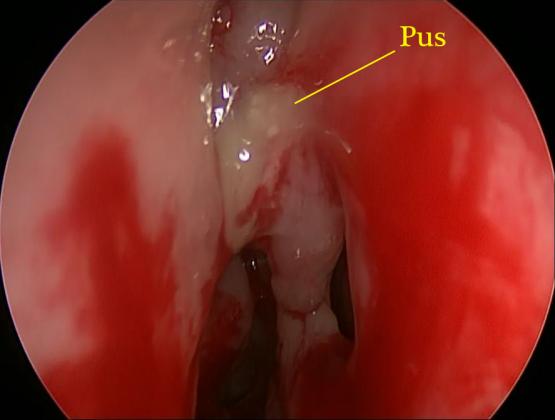 In addition to these symptoms, your doctor may see evidence of sinus or nasal inflammation, purulent (pus-containing) mucus, or nasal polyps on examination or with imaging studies such as a CAT scan.
In addition to these symptoms, your doctor may see evidence of sinus or nasal inflammation, purulent (pus-containing) mucus, or nasal polyps on examination or with imaging studies such as a CAT scan.
There are numerous causes of chronic rhinosinusitis including infectious (viral, bacterial, and fungal), allergic, anatomic, mucociliary (a problem with the natural clearance mechanism of the sinuses such as in cystic fibrosis or ciliary dyskinesia), and systemic disorders. Chronic rhinosinusitis is typically further subdivided into categories of patients with and without polyps.
Treatment:
Depending on the severity and duration – sinus infections are usually treated with medical therapy first. This can consist of over the counter decongestants, antihistamines, and nasal saline sprays. When these are ineffective, oral antibiotics and/or steroids are usually necessary. Certain patients will also benefit from topical steroids in the form of steroid sprays or medicated nasal irrigations. Topical antibiotics are also effective when used on the correct patient and when culture directed. When these more conservative measures are not successful and sinusitis persist or complications arise, in office procedures or surgery may be recommended by your physician.
 The paranasal sinuses are air-filled extensions of the nasal cavity. They are located in the face/skull and connect directly or indirectly to the nasal cavity and nose through narrow drainage pathways. The frontal sinuses (purple) are located in the forehead region, the ethmoid sinuses (blue) are located between the nasal septum and the eye and just below the brain, and the maxillary sinuses (green) are located in the cheek region below the eyes. The sphenoid sinuses (red) are located behind the ethmoid sinuses and are closely related to important anatomical structures such as the optic nerves that are required for vision, the pituitary gland, and the carotid arteries that carry blood to the brain.
The paranasal sinuses are air-filled extensions of the nasal cavity. They are located in the face/skull and connect directly or indirectly to the nasal cavity and nose through narrow drainage pathways. The frontal sinuses (purple) are located in the forehead region, the ethmoid sinuses (blue) are located between the nasal septum and the eye and just below the brain, and the maxillary sinuses (green) are located in the cheek region below the eyes. The sphenoid sinuses (red) are located behind the ethmoid sinuses and are closely related to important anatomical structures such as the optic nerves that are required for vision, the pituitary gland, and the carotid arteries that carry blood to the brain.

 In addition to these symptoms, your doctor may see evidence of sinus or nasal inflammation, purulent (pus-containing) mucus, or nasal polyps on examination or with imaging studies such as a CAT scan.
In addition to these symptoms, your doctor may see evidence of sinus or nasal inflammation, purulent (pus-containing) mucus, or nasal polyps on examination or with imaging studies such as a CAT scan.